Chinese Journal of Tissue Engineering Research ›› 2013, Vol. 17 ›› Issue (51): 8841-8848.doi: 10.3969/j.issn.2095-4344.2013.51.010
Previous Articles Next Articles
Comparison of magnetic attachment and ball-cap attachment for retained mandibular over-denture
Yao Xi1, Li Yun-sheng1, Dai Yong-yu2
- 1 Department of Stomatology, China Meitan General Hospital, Beijing 100028, China
2 Department of Stomatology, Beijing Hospital of Health Ministry of China, Beijing 100730, China
-
Online:2013-12-17Published:2013-12-17 -
About author:Yao Xi★, Master, Attending physician, Department of Stomatology, China Meitan General Hospital, Beijing 100028, China yaoxi_heather@163.com
CLC Number:
Cite this article
Yao Xi, Li Yun-sheng, Dai Yong-yu. Comparison of magnetic attachment and ball-cap attachment for retained mandibular over-denture[J]. Chinese Journal of Tissue Engineering Research, 2013, 17(51): 8841-8848.
share this article
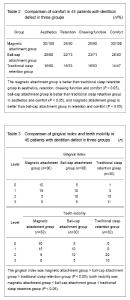

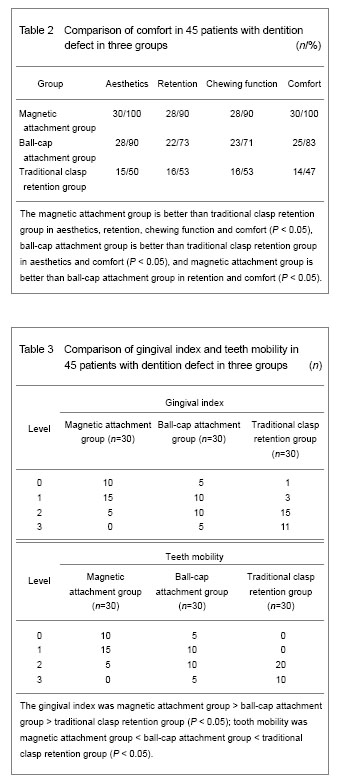
Satisfaction survey After precision attachment of overdenture restoration, patients were highly satisfied in the aesthetics, denture retention, chewing function and comfort compared with traditional clasp retention of removable partial denture. (1) Aesthetics: There were significant differences between magnetic attachment group and control group (χ2=14.892, P=0), and between ball-cap attachment group and control group (χ2=13.871, P=0). This evidence suggested that, the appearance of two precision attachments was better than clasp retainer. No difference was significant between magnetic attachment group and ball-cap attachment group (χ2= 2.069, P=0.246). (2) Retention: There were significant differences between magnetic attachment group and control group (χ2=12.273, P=0), which indicated that magnetic attachment was better than traditional clasp retainer in the denture retention. There was no significant difference between ball-cap attachment group and control group (χ2=2.584, P=0.180), and between magnetic attachment group and ball-cap attachment group (χ2=4.320, P=0.040). This evidence suggested that patients in magnetic attachment group and ball-cap attachment group were satisfied in the retention. (3) Chewing function: There were significant differences between magnetic attachment group and control group (χ2=12.273, P=0), which indicated that magnetic attachment was better than traditional clasp retainer in the chewing function. There was no significant difference between ball-cap attachment group and control group (χ2=3.590, P=0.103), and between magnetic attachment group and ball-cap attachment group (χ2=3.268, P=0.073). The traditional clasp retention group and magnetic attachment group showed no significant difference compared with ball-cap attachment group. (4) Comfort: There were significant differences between magnetic attachment group and control group (χ2=21.818, P=0), and between ball-cap attachment group and control group (χ2=8.864, P=0.006), suggesting that two precision attachments were more comfortable than clasp retainer. No difference was significant between magnetic attachment group and ball-cap attachment group (χ2=5.455, P=0.026), suggesting that the comfort was more apparent in magnetic attachment and ball-cap attachment group (Table 2). Periodontal health Gingival index and teeth mobility The gingival health in magnetic attachment group was better than ball-cap attachment group (P=0.006); and two attachment groups were better than control group (P=0). The abutment tooth mobility in magnetic attachment group was lower than ball-cap attachment group (P=0); two attachment groups were both lower than control group (P=0; Table 3)."
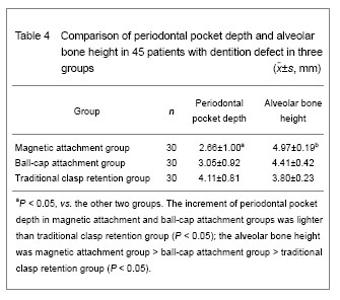
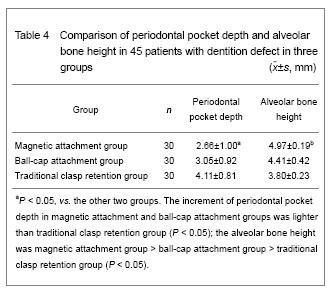
Periodontal pocket depth and alveolar bone height Periodontal pocket depth was measured by clinical probing methods. In brief, each tooth surface was detected using a periodontal probe along the tooth long axis, the probing depth in each tooth was measured at six locations, including the cheek (lip) and tongue levels at the distant, central, and proximal side respectively, then the average value was obtained[5]. At 3 years after treatment, the periodontal pocket depth of all patients was statistically analyzed and the results showed that the depth was slightly increased in two attachment groups without significant differences (P=0.126). The increment in magnetic attachment group and ball-cap attachment group was lower than the control group (P=0.007, P=0.040; Table 4). Alveolar bone height was detected using panoramic X-ray by measuring the distance from mandibular alveolar ridge to mandibular inferior margin[5]. Statistical analysis of clinical measurement results showed that alveolar bone height in magnetic attachment group was higher than ball-cap attachment group and control group (P=0), and ball-cap attachment group was higher than control group (P=0; Table 4)."
| [1]Zhu HW. Clinical effect of study Ball-cap attachments in the rehabilitation of dentition free deletion based on the treatment of 37 patients suffering from severe periodontal disease. Zhongguo Shiyong Kouqiangke Zazhi. 2011;4(7): 433-434.[2]Boeckler AF, Morton D, Ehring C. Mechanical properties of magnetic attachments for removable prostheses on teeth and implants. J Prosthodont. 2008;17(8):608-615.[3]Zinner ID, Miller RD, Panno FV. Clinical management of abutments with intracoronal attachments. J Prosthet Dent. 1992;67(6):761.[4]State Council of the People’s Republic of China. Administrative Regulations on Medical Institution. 1994-09-01.[5]Cao CF. Periodontology. Beijing: Renmin Weisheng Chubanshe. 2001:87,90,94.[6]Liu W. Effect observation of the curative effect of magnetic attachment in mandibular denture. Xiandai Yiyao Weisheng. 2010;26(6):849-850.[7]Jiang Y, Liu HC, Li HB, et al. Application of single complete overdenture with magnetic attachments in the elderly. Kouqiang Hemian Xiufuxue Zazhi. 2012;13(2):79-82.[8]Wu XX, Zhang XM, Zhang Y, et al. Clinical application of Magnetic attachment in restoration of removable partial denture. Zhonghua Laonian Kouqiang Yixue Zazhi. 2009; 7(1):39-41.[9]Wang PZ, Xia L, Wang GP, et al. Clinical effects of complete mandibular overdenture with magnetic attachments. Kouqiang Hemian Xiufuxue Zazhi. 2005;6(2):121-123.[10]Wu LJ, Wang X, Zhang GY. Clinical research of complete mandibular overdentures with magnetic attachments. Kouqiang Yixue. 2010;30(2):103-105.[11]Vere J, Deans RF. Tooth-supported, magnet-retained overdentures: a review. Dent Update. 2009;36(5):305-308, 310.[12]Zheng XJ, Wei HW, Huang JJ. Magnetic precision attachment in mandibular denture in the coverage application. Shiyong Linchuang Yixue. 2010;11(6): 90-91.[13]Zhu S. Clinical observation of body overdenture elderly edentulous magnetic attachment. Kouqiang Yixue. 2010;30(9):571-572.[14]Tsuchida F, Suminaga Y, Takishin N, et al. A new retainer using magnetic attachment.Nihon Hotetsu Shika Gakkai Zasshi. 2008;52(4):559-561.[15]Preiskel HW, Preiskel A. Precision attachments for the 21st century.Dent Update. 2009;36(4):221-224, 226-227.[16]Zeng D, Jiao LP, Liu G, et al. Clinical evaluation of magnetic attachment retained over-denture and traditional removable partial denture. Kouqiang Hemian Xiufuxue Zazhi. 2010; 3(11):84-86.[17]Zeng D, Jiao LP, Liu G, et al. Clinical observation of magnetic attachment overdenture restoration for patients with advanced periodontitis. Zhonghua Laonian Kouqiang Yixue Zazhi. 2010;8(2):88-92.[18]Liu LY, Jiang T, Feng HL. Fatigue test of retention force of magnetic attachment and stud-type attachment. Shiyong Kouqiang Yixue Zazhi. 2008;24(5):635-638.[19]Kuang H, Wang H, Huang XH, et al. Magnetic attachment for observation of the elderly's dentition defect repair effect. Gannan Yixueyuan Xuebao. 2012;32(2):218-219.[20]Xiong YR, Feng D, Pang JL. Clinical application of magnetic attachments in complete overdentures in elder patients. Zhongguo Zuzhi Gongcheng Yanjiu. 2012; 16(12):2273-2276.[21]Li MJ, Liu AG. Clinical application and common problems of magnetic attachment of overdenture. Gguangdong Yabing Fangzhi. 2010;18(8):443-446.[22]Zhong AX, Pan XB, Peng LH, et al. Clinical application of SD ball attachment dentures. Guangxi Yike Daxue Xuebao. 2008;25(6):904-905.[23]Deng SN. Comparative study of masticatory efficiency between attachment dentures and clasp removable partial dentures. Xiandai Yiyao Weisheng. 2008;24(10): 1459-1461.[24]Saito M, Miura Y, Notaniet K, et al. Stress distribution of abutments and base displacement with precision attachment- and telescopic crown-retained removable partial dentures. J oral Rehabil. 2003;30(5):482-487. |
| [1] | Su Tingshu, Tang Ying, Sun Jian. Application of intraoral scanning and 3D printing in the manufacture of removable partial dentures [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(4): 544-548. |
| [2] | Chen Junliang, Li Mingxia, Lü Dongmei, He Yun. Three-dimensional finite element analysis of mini implants supported mandibular overdentures [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(10): 1491-1495. |
| [3] | Pang Guobao, Zhao Ning, An Meiwen. Effect of relative position of planting denture on interdental food impaction: finite element analysis [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(10): 1521-1527. |
| [4] | Luo Heng, Gao Hai, Xu Xuefei, Feng Yunzhi. Preparation, water absorption and solubility of a new Eucommia ulmoides gum composite soft denture liner [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(10): 1501-1506. |
| [5] | Wang Zhong-da, Wang Yi-bo, Ding Chao, Shi Jiu-hui. Three-dimensional finite element analysis of implant denture for anterior tooth missing with different arch shapes [J]. Chinese Journal of Tissue Engineering Research, 2018, 22(30): 4818-4823. |
| [6] | Long Yan-ming, Li Xiao-jie . Types and properties of injection-molded thermoplastic denture base resins [J]. Chinese Journal of Tissue Engineering Research, 2018, 22(14): 2278-2283. |
| [7] | Shan Jian-liang, Zhang Qin, Hu Yang, Yao Yuan, Zhang Wei, He Hui-yu. Effect of osteoporosis on the prognosis of implant dentures [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(4): 586-590. |
| [8] |
Tang Zhen-yu, Zhang Zhe, Zhang Wei-yi.
A comparative study on the mechanical properties of flexible denture materials containing different fluoride concentrations
[J]. Chinese Journal of Tissue Engineering Research, 2017, 21(30): 4805-4810.
|
| [9] |
Xue Wen-li, Li Xiao-jie .
Advances and clinical application in digital complete denture
[J]. Chinese Journal of Tissue Engineering Research, 2017, 21(26): 4258-4264.
|
| [10] |
Yu Tian-hao, Jia Xing-ya, Xue Yan-qing, Zhan De-song, Yan Xu.
Correlation between complete denture relines and serum bone turnover markers in elderly edentulous patients with osteoporosis
[J]. Chinese Journal of Tissue Engineering Research, 2017, 21(22): 3513-3518.
|
| [11] |
Li Ting, Sun Jun, Xu Deng-you, Mo Wen-juan, Lin Bao-shan.
Effects of denture cleansers on color stability and surface roughness of heat-curing denture base resins and elastic denture base materials
[J]. Chinese Journal of Tissue Engineering Research, 2017, 21(18): 2814-2820.
|
| [12] | Zhang Qiang, Zhang Yu, Xie Chang. Investigation on patient satisfaction with single or bridge crown for repair of consecutive missing posterior teeth in the maxilla [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(14): 2203-2207. |
| [13] | Zhou Jing, Ye Xiang, Zhu Xiang-dong, Jiang Xue-hua. Current situation of customised denture manufacturing enterprises in Sichuan, China [J]. Chinese Journal of Tissue Engineering Research, 2016, 20(47): 7133-7138. |
| [14] | Gao Shi-jun, Ren Guo-xin, Wei Si-yi, Chu Ming-hui, Wang Dong-xia, Hou Yu-ze, Xiao Yuan-yuan, Huang Yan-jun, Jiang Jia-zhen. Effect of anhydrous calcium sulfate whisker on the mechanical function of soft denture liners [J]. Chinese Journal of Tissue Engineering Research, 2015, 19(47): 7624-7628. |
| [15] | Ma Guo-lan. Different application ways of binders influence the bonding performance of total-etch resin cements with the dentin [J]. Chinese Journal of Tissue Engineering Research, 2015, 19(47): 7634-7638. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||